Dr. Weeks’ Comment: Meta analysis (resifting the results from many studies) is a new trend in computer-aided refocusing of causality which, like the childhood game of “Telephone”, removes us increasingly from the actual reality behind the questions being asked. In the case of the merits of omega 3 fatty acids for people with prostate cancer, neither of those variables were scrutinized directly and a careful analysis of this publication shows sloppy science at best and undeclared bias with conflict of interest at worse. Furthermore, the big news of this predictably well-publicized negative study flies in the face of hundreds of actual research papers on the topics. As always, friends, follow the money and remember that Big Pharma would like to capture the billions spent by you and me and other informed American who buy nutritional supplements to correct imbalances in order to steer those funds into their own multinational coffers by having us buy synthetic, patented drugs rife with negative side-effects. In order to accomplish that, “research” needs to show no benefit or perhaps some harm derives from supplements. This article represents only the more recent in a concerted campaign of dis-information masquerading as science. The solution? Eat organic fish and take top quality nutritional supplements but take them as a SUPPLEMENT to corrective lifestyle which incorporates healthy exercise, sleep, diet and a purpose- filled life. Supplements are supplemental to lifestyle and you need to see these meta smear jobs for what they are – paid for propaganda by shills who trade on their academic credentials in the service of Big Pharma.
On July 10, 2013, major media headlines and news stories claimed “Too Much Fish Oil Might Boost Prostate Cancer Risk.” Wow, that sure seems fishy given all of the positive health benefits linked to fish oil intake. In examining the study, there are numerous issues that clearly indicate that perhaps the conclusion is wrong, but really a study’s conclusion is only as good as the study itself.
Data Used was From the SELECT Study
The pedigree of the study source is impressive. It was published in the Journal of the National Cancer Institute and was conducted by researchers from the Fred Hutchinson Cancer Center in Seattle, WA.1 Yet, the data they used is from the much maligned Selenium and Vitamin E Cancer Prevention Trial (SELECT). That is the real problem.
The SELECT study was a very large clinical study that attempted to determine whether vitamin E could prevent prostate cancer. Previous studies had shown 50 IU of vitamin E was protective against prostate cancer, but the SELECT study chose to use 400 IU of synthetic vitamin E (dl-alpha-tocopherol) at a dosage of 400 IU. Results showed that the subjects taking vitamin E alone had a 17% higher risk of prostate cancer compared to the control group.
In the new analysis, researchers measured the levels of fats in the blood (plasma phospholipids) and concluded that men with the highest concentrations of EPA, DPA and DHA-three fatty acids derived from fish and fish-oil supplements-had an increased risk of prostate cancer. Specifically, they reported a 71 percent increased risk of high-grade prostate cancer; a 44 percent increase in the risk of low-grade prostate cancer and an overall 43 percent increase in risk for total prostate cancer in a subset of patients with the highest level of these omega-3 fatty acids.
Important considerations of this data are the following:
- This study is not consistent with other studies (discussed below)
- The study did NOT include information or documentation of fish or fish oil intake in the study group. It was NOT set up initially to evaluate these factors, hence its relevance is not as significant as studies designed to specifically determine the impact of omega-3 fatty acids on prostate cancer risk.
- There is no evidence that anybody in this study took fish oil supplements or even ate fish.
- In usual circumstances, plasma levels of EPA and DHA reflect very recent intake and are considered a poor biomarker of long-term omega-3 intake.
- Patients with prostate cancer may have only recently increased their fish and/or fish oil consumption.
- Fish and fish oil ingestion produces a big rise in plasma omega-3 levels in about 4.5 hours and washes out around 48 hours.
- The data may reflect cancer activity rather than a causative association. Without dietary history or documentation of fish oil use there is no way of knowing.
Lastly, the following statement by the authors suggests that they may have significant bias: “There is really no evidence that taking dietary supplements is beneficial to health, and there is increasing evidence that taking high doses is harmful.” Such a statement shows a clear axe to grind in light of a great deal of scientific evidence on the value of dietary supplementation.
A Closer Look at the Reported Results
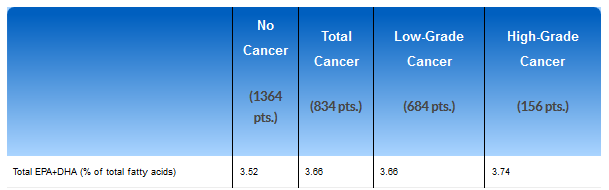
Let’s take a closer look at the reported results to see if things add up. The bottom line is that they do not. Let’s first take a look at the blood levels of EPA+DHA – the major forms of long-chain omega-3 fatty acids found in fish oil supplements. As Table 1 shows the levels are quite similar among the groups. These blood levels of EPA+DHA are actually quite modest and do not reflect huge levels of fish or fish supplements being consumed. The average EPA+DHA plasma level for men is generally approximately 4%. So, the levels reported here are typical, but a little lower than normal and the ratio of EPA to DHA is also a little lower as well.
Table 1. Distribution of EPA and DHA among SELECT participants by prostate cancer grade (n=2273)*
That the researchers did next was divide cancer patients up by their blood levels of fatty acids and look at the hazard ratio – the relative risk over time – associated with different levels of the various fatty acids (see Table 2). As it relates to EPA, statistical significance was not achieved for total cancer or high-grade cancer (the P value has to be less than 0.05 to be deemed anything more than random chance). For DHA, there was statistical significance. But, again, the levels of DHA are typical of what is found in men consuming modest amounts of fish. However, the level of EPA was lower than that typically found and the ratio of EPA to DHA was also lower. What this may mean is that there may be increased conversion of EPA to DHA in prostate cancer. Though one interesting observation is that the hazard ratio (HR) actually went down in high-grade prostate cancer in the group with the highest level of DHA compared to the next highest group. This suggests that it is not that significant of a factor as one would expect if it was that the higher the level the higher the HR. But, this finding has a P value of 0.09 so no real conclusions can be made as it was probably a random finding.
Table 2. Associations between EPA and DHA among SELECT participants by prostate cancer grade (n=2273)
The authors conclude that men are at higher risk of aggressive prostate cancer if the total plasma level of long-chain omega-3 fatty acids (EPA+DPA+DHA) is greater than 3.68%. If that were true, then aggressive prostate cancer would be a major health concern and the leading cause of death in any country with even moderate fish consumption. The facts are that population-based studies show just the opposite effect. For example, prostate cancer incidence and death rates are among the lowest known in populations consuming the traditional Japanese or Mediterranean diets, two diets with a relatively high content of EPA+DHA.
What do other Studies Show?
In addition to population-based studies, several studies have been conducted that were actually designed to determine the effects of fish and fish oil consumption in prostate cancer. In a detailed meta-analysis conducted in 2010, while fish consumption did not affect prostate cancer incidence, it was associated with a 63% reduced mortality due to prostate cancer.2 A meta-analysis examines all previously conducted studies. Here are some of the results from some of these studies:
- Researchers investigated the effect of dietary fatty fish intake among 6,272 Swedish men who were followed for 30 years. Results showed that men who ate no fish had a two- to three-fold increase in the risk of developing prostate cancer compared with those who consumed large amounts of fish in their diet.3
- Data from the Physician’s Health Study, a study spanning 22 years, found that fish consumption (≥5 times per week) reduced the risk of dying from prostate cancer by 36%.4 -specific death.
- A study conducted by the Harvard School of Public Health that involved 47,882 men over twelve years found that eating fish more than three times a week reduced the risk of prostate cancer but had an even greater impact on the risk of metastatic prostate cancer. For each additional 500 mg of marine fat consumed, the risk of metastatic disease decreased by 24%.5
- In one of the best-designed studies, researchers in New Zealand examined the relationship between prostate cancer risk and EPA+ DHA in red blood cells (a more reflective marker for long-term omega-3 fatty acid intake). Higher levels of EPA+DHA were associated with a 40% reduced risk of prostate cancer.6
- In a study of 47,866 US men aged 40-75 years with no cancer history in 1986 who were followed for 14 years EPA+DHA intake at the highest levels was associated with a 26% reduced risk of developing prostate cancer.7
While some studies make an important distinction, others do not. When ascertaining the benefits of fish consumption it is important to find out how the fish is being prepared. For example, regular ingestion of fried fish was associated with a 32% increased risk for prostate cancer.8 In addition, many studies do not control for the quality of fish or fish oil. Some fish (and fish oil supplements) can contain environmental chemicals that can contribute to prostate cancer such as PCBs, heavy metals, and other toxic chemicals.9, 10 These are important considerations.
Final Comments
The best thing about this study is that it will stimulate more research into the role of omega-3 fatty acids in prostate health. The worst thing about this study is that it may lead to many men abandoning the use of fish oil supplements. Based upon a large amount of clinical data it makes sense for men to be consuming 1,000 mg of EPA+DHA daily for general health. And, if they are suffering from one of the over 60 different health conditions shown to be benefitted by fish oil supplementation the dosage should be increased to 3,000 mg of EPA+DHA daily.
References:
1. Brasky TM, Darke AK, Song X, et al. Plasma phospholipid fatty acids and prostate cancer risk in the SELECT Trial. J National Cancer Inst Online. July 10, 2013 doi: 10.1093/jnci/djt174
2. Szymanski KM, Wheeler DC, Mucci LA. Fish consumption and prostate cancer risk: a review and meta-analysis. Am J Clin Nutr. 2010 Nov;92(5):1223-33.
3. Terry P, Lichtenstein P, Feychting M, Ahlbom A, Wolk A. Fatty fish consumption and risk of prostate cancer. Lancet 2001; 357: 1764-6
4. Chavarro JE et al. A 22-y prospective study of fish intake in relation to prostate cancer incidence and mortality. Am J Clin Nutr 2008; 88: 1297-303.
5. Augustsson, K., et al., A prospective study of intake of fish and marine fatty acids and prostate cancer. Cancer Epidemiol Biomarkers Prev, 12(1): p. 64-7, 2003.
6. Norrish AE, Skeaff CM, Arribas GL, Sharpe SJ, Jackson RT. Prostate cancer risk and consumption of fish oils: a dietary biomarker-based case-control study. Br J Cancer 1999;81:1238-42.
7. Leitzmann MF, Stampfer MJ, Michaud DS, et al. Dietary intake of n-3 and n-6 fatty acids and the risk of prostate cancer. Am J Clin Nutr. 2004 Jul;80(1):204-16.
8. Stott-Miller M, Neuhouser ML, Stanford JL. Consumption of deep-fried foods and risk of prostate cancer. Prostate. 2013 Jun;73(9):960-9.
9. Ritchie JM, Vial SL, Fuortes LJ, Robertson LW, Guo H, Reedy VE, Smith EM.Comparison of proposed frameworks for grouping polychlorinated biphenyl congener data applied to a case-control pilot study of prostate cancer. Environ Res. 2005;98(1):104-13.
10. Mullins JK, Loeb S. Environmental exposures and prostate cancer. Urol Oncol. 2012 Mar-Apr;30(2):216-9.